James DiNicolantonio’s book The Salt Fix first crossed my radar when my wife forwarded me the article When Salt Restriction Backfires, which referenced this book and claimed that our low-salt diet might be contributing to her hypothyroidism. How? As the argument went, less salt ⇨ less chloride ⇨ less hydrochloric acid (stomach acid) ⇨ less digestion of key nutrients required for thyroid function ⇨ more hypothyroidism, which is of course not good. The theory seemed intriguing. So, trying to keep an open mind, off I went to read The Salt Fix.
The book’s core message is this: salt is good for you. So good, in fact, that you shouldn’t eat any less of it no matter what the vast majority of experts and health organizations may have told you—such as the low-salt diet recommended by the American Heart Association that limits sodium to 1,500 mg per day. Instead, you should probably eat even more of it—a high-salt diet with somewhere between 3,000 and 5,000 mg of sodium per day.
Let’s be clear: nobody disputes the fact that sodium and chloride (which together make up salt) are essential nutrients that support various key processes in our bodies, including regulating blood pressure. The question is this: what amount of sodium is healthy? Can too little make you just as sick as too much? And how much is too much? Therein lies the heart of a debate that has been raging on for around a hundred years.
Most readers don’t have time to fact-check the dozens of claims the author makes. But I did. And I felt that it would be in the public interest for me to invest that time (about three weeks of in-depth research) and share what I have found with you. As it turns out, this is more than just a review of one book—this is really a review of the plethora of arguments that the salt industry has been conjuring over the years to exonerate their product from the criticisms of thousands of health experts.
Without further ado, let’s dive into The Salt Fix’s claims one by one. How many of them will stand up to scrutiny?
Table of contents
First things first:
Does a low-salt diet …
…increase renin, angiotensin, and aldosterone, leading to heart failure and kidney disease?
…reduce sex drive and fertility, and increase erectile dysfunction?
…cause Yanomamo aboriginals to have a low birth rate?
…lead to an insignificant drop in blood pressure?
…provide no benefits and possibly some harms, according to the 2013 IOM report?
…cause you to absorb twice as much fat?
…cause nonalcoholic fatty liver disease?
…cause drug and food addiction?
…during pregnancy produce children that crave salt?
…during pregnancy lead to health issues in offspring?
…cause anxiety, hypochondriasis, and invalidism?
…like the ultra-low-sodium Rice Diet, dangerously deplete chloride?
…like the ultra-low-sodium Rice Diet, fail to reduce blood pressure in most patients?
Did our ancient ancestors consume a high-salt diet because …
…they ate fish and aquatic plants?
…Australian Aborigines ate a lot of meat?
Is the other white crystal (sugar) the real bad guy?
Do sugar and salt help us to eat more healthy food?
Does refined sugar and salt encourage us to eat healthy foods?
Does refined sugar, not salt, stimulate reward centers like drugs do?
Is sodium intake across countries correlated with hypertension and cardiovascular disease?
Does the 1988 Intersalt study show that higher-salt diets lower blood pressure?
Do some countries consume a high-salt diet yet have fewer heart disease deaths?
Does South Korea have low rates of hypertension despite a high salt intake?
Is sodium intake across history inversely related to heart disease?
Historically, is salt intake inversely related to heart disease?
Did Americans eat less salt after the invention of refrigerators?
Instead of reducing salt, can’t we instead solve hypertension by …
Is a high-salt diet …
…much easier to follow than a low-salt diet?
…able to increase metformin’s effectiveness?
…able to prevent hyponatremia?
…what the human body is best adapted to, via several mechanisms?
What about these specific situations?
Does exercise cause sodium sweat losses of 2g per hour?
Does hypothyroidism lead to hyponatremia (low blood sodium)?
Do older adults have a reduced ability to retain sodium, thus needing to consume more of it?
Controversial trials and other considerations:
Claim: “Scientists have found that across all populations, when people are left to unrestricted sodium consumption, they tend to settle in at 3,000 to 4,000 milligrams of sodium per day. This amount holds true for people in all hemispheres, all climates, all range of cultures and social backgrounds—when permitted free access to salt, all humans gravitate to the same threshold of salt consumption, a threshold we now know is the sodium-intake range for optimal health.” He calls this a built-in “salt thermostat” or “salt set point” that regulates our salt intake automatically, “without any effort on our part.”
Fact check: If we all had a “salt thermostat” that precisely regulated our salt intake, there wouldn’t be such a wide variability in consumption across the world and throughout history. According to the Global, regional and national sodium intakes in 1990 and 2010 report, estimated average sodium intakes ranged from around 1,600mg/day in Rwanda to nearly 6,000mg/day in Kazakhstan. Other estimates are even higher—according to the WHO, Turkey’s sodium consumption in 2008 was as high as 7,200mg/day based on 24h urine collections (the gold standard for sodium consumption estimates) but dropped to around 6g/day in 2012 after the government instituted a salt-reduction program. Keep in mind that these are national averages—regional averages will likely exhibit even larger variations. Case in point: northern Japan once averaged over 10g/day. DiNicolantonio himself claims on p.32 that eighteenth century Europeans consumed up to a whopping 70 grams of salt daily (that’s 28,000mg of sodium). All of which seem to contradict his proposition that humans naturally and effortlessly settle on a narrow daily range of 3,000 to 4,000mg.
Even more critical is the fact that, prior to the deliberate mining of salt a few thousand years ago, our ancestors simply did not have “free access to salt”—none of them had salt shakers or pre-salted processed foods. Granted, a minority may have lived near a salt lick and used it, which we’ll discuss later. But why would the vast majority of our ancient ancestors evolve a preference for a sodium range that is only achievable with free access to salt, when they themselves did not have free access to salt? 🤔 Hmmm…
Furthermore, this argument presumes that we are hard-wired for a fixed, narrow range of sodium that is guided by our taste buds. However, the author himself states (on p.102) that we can adapt to different levels of sodium: “If you habitually add salt to your food, the worst that could happen is that your taste buds get used to that level of saltiness.” According to research by Michael J Morris, then at the University of Iowa, there is evidence that we tend to be born with indifference or even aversion to moderate- or high- salt foods, but that we adapt to them after a period of exposure—and then find it hard to go back to a lower-salt diet. But the opposite is also true: Gary Beauchamp, director of the Monell Center whose research focus is taste and scent, carried out a study that showed that after about four to eight weeks on a low-sodium diet, the amount of salt that participants found optimal in soup or crackers went down by nearly 50%. When those individuals re-tasted the higher-salt foods of their former diet, they now found them too salty. Bottom line: our taste buds can adapt to both higher and lower sodium diets, given enough time.
Claim: A low-salt diet increases insulin and can cause insulin resistance.
Fact check: This paper reviewed all studies up through 2015 that examined the impact of reduced sodium on insulin resistance. They noted that studies of a short duration tended to find either no change or an increase in insulin resistance. On the other hand, those lasting longer than four weeks were more likely to find a decrease in insulin resistance. As such, the body’s insulin mechanisms seem to take a few weeks to adapt to a lower-salt diet (which seems to be the case for other biomarkers including blood pressure, as we’ll see below).
Claim: A low-salt diet increases levels of renin, angiotensin, and aldosterone (the RAAS system), which might actually lead to heart failure and kidney disease.
Fact check: This 2016 meta-analysis of 74 studies concluded that “although renin activity is increased in the early phase of sodium intake restriction,” the renin levels reduced over time and returned to around their baseline levels after about a month. “Thus, it seems very unlikely that activation of RAAS in the early phase of sodium intake restriction persists and contributes the development of CVD [cardiovascular disease].”
Furthermore, this 2020 meta-analysis of 133 studies concluded that “The responses of the renin-angiotensin system and sympathetic nervous system as well as adverse metabolic effects associated with acute large falls in dietary sodium do not, however, appear to be present in longer term interventions and it is unlikely that short term unfavourable metabolic effects would override the long term benefits anticipated from sustained blood pressure lowering of moderate magnitude.”
Again, it seems to take a few weeks for our RAAS system to adapt to a lower-salt diet.
Claim: Despite the majority of scientists believing that our evolutionary ancestors evolved on a low-salt diet, we actually evolved on a high-salt diet. One line of evidence is that some modern-day primates eat fish and aquatic plants.
Fact check: His own source noted that about 20 nonhuman primate species have been observed eating aquatic fauna, specifically fish. However, there are 190-350 species of primates (depending on whose taxonomy you use). Thus only 5 to 10% of extant nonhuman primates actually appear to eat fish or seafood. Furthermore, the primates in the above paper were orangutans that were observed only eating disabled catfish, primarily in the dry season. The authors described fish-eating as “rare” and “novel” for nonhuman primates, which primarily eat plants and invertebrates.
It is true that plain fish, like other animal foods, do contain more sodium than fruits and vegetables, but not as much as one may think. According to Seafood Health Facts, a multi-university initiative, “Fish are naturally low in sodium and even those species with the highest sodium levels contain less than 100 milligrams per 3 ounce [85g] cooked portion.” Even if you only ate cod all day long (54mg sodium and 82 calories per 100g serving), a 2400-calorie diet would yield 1,580mg sodium a day—less than half of the “official” American average intake of 3,400mg/day (though some contend that the true average is closer to 4,000mg/day).
That said, I was honest-to-goodness shocked to learn that shellfish can contain a much higher amount of sodium, quite possibly the highest of all natural, unprocessed foods: “Most shellfish generally have more sodium, ranging from 100 to 500 milligrams per 3 ounce cooked serving,” according to Seafood Health Facts. The saltiest seafood I could find in the USDA database that wasn’t obviously battered or fried was king crab at a whopping 1,000mg of sodium per 100 calories. However, many sources say that crustaceans (like crabs) are often brined upon harvesting and again upon freezing. This makes it hard to tell how much of the sodium is naturally occurring versus added by humans. Nevertheless, if all you ate were uber-salty king crabs day in, day out, a 2500-calorie diet would yield an astronomical 25,000mg of sodium.
Bottom line: it seems possible to eat a very high-sodium diet with natural foods, but only if you eat a lot of high-sodium shellfish. However, no evidence is provided to suggest that ancient humans ate a shellfish-heavy diet.
Claim: Another line of evidence that we evolved on high-salt diets is that our purported ancestor, the so-called Nutcracker Man, ate a diet high in tiger nuts and that these contain up to a whopping 3,300mg sodium per 100g serving.
Fact check: While his source does state that one sample of tiger nuts (a kind of tuber) bought at a Nigerian market were indeed that high in salt, every other source of nutrition information on tiger nuts that I consulted contained vastly less sodium—all under 10mg per 100g serving. Furthermore, having read thousands of nutrition facts labels for all kinds of processed and unprocessed foods over the years, I have never in my life seen any plant-based food remotely as high in sodium as the cited tiger nuts. The most rational explanation? That these tiger nuts had been heavily salted prior to being packaged and sold—or that the scientists’ sodium assay method was somehow faulty.
I also find it interesting that, out of the thousands of plant based foods our ancestors may have eaten, DiNicolantonio zeroed in on the one outlier that tested astronomically high in sodium.
Beyond this, a 2008 analysis of the Nutcracker Man’s teeth concluded that they ate mostly soft foods like fruit, as opposed to nuts or other hard, abrasive items.
(P.S. The Nutcracker Man doesn’t even appear to be a direct ancestor of Homo sapiens—Thanks Matthew Dalby for pointing this out!)
Claim: As further evidence that we evolved on high-salt diets, he states that “muscle contains approximately 1,150 milligrams of sodium per kilogram. Australian Aborigines would eat 2 to 3 kilograms of meat per sitting during a kill. This is equal to 3,450 milligrams of sodium per day, the exact amount of sodium that current-day Americans consume”.
Fact check: Three sentences, three arguably incorrect statements:
1. He implies that these Aborigines ate 3kg of meat each day, but the cited article clearly states that “Aborigines from all over Australia were omnivores” and had a diet high in fiber—in other words, high in plant-based foods. The article further describes this amount of meat-eating as “gorging” and that meat was only “episodically available.”
2. He implies that 3kg of meat is an achievable daily intake. The problem is that even if you threw all your veggies out the window and ate just meat (something that virtually no health organization recommends), a typical 2500-calorie diet would only amount to between 1 and 1.5kg of meat a day, depending on the type of meat and its fat content (see the USDA nutrition data for plain chicken breast, ground beef with 30% fat, and ground beef with 5% fat).
3. He asserts that muscle contains 1,150mg sodium/kg, but does not back up this number with a source. In contrast, the USDA indicates that plain chicken breast and ground beef contain only 470-730mg sodium/kg. Based on what are arguably the two most popular (plain) meats consumed in North America, his stated “1,150mg sodium/kg” figure appears inflated by roughly 50% to 150%.
Has DiNicolantonio made a series of honest mistakes, or has there been a deliberate manipulation of facts in order to achieve the desired end target of 3,450mg/day sodium, which is precisely the amount that the average American currently eats? Hmmm… 🤔
The final nail in the coffin of this particular claim: his own reference describes the Aborigines as having a “low sodium but high potassium magnesium and calcium intake” that “protected against obesity, non insulin dependent diabetes and cardiovascular diseases.” (emphasis mine)
Claim: “Early humans probably got salt in other ways as well. Some would have also eaten soil, as is still done by Kikuyu women of Africa, who are known to make dishes from sodium-rich soil.”
Fact check: Soil and clay do contain a variable amount of sodium, but it’s unclear how much of these our ancestors would have eaten. Some African countries do practice clay eating either out of tradition, or out of belief it has special nutritive properties, or simply because they can’t afford real food. Many commercial, edible clays have salt added to them, such that the majority of their sodium content is not naturally occurring. But doctors want this practice to stop because it tends to cause intestinal blockages, parasitical infections, and may actually interfere with the absorption of minerals. It does not appear that clay-eating is particularly health-promoting—except perhaps for occasional, small amounts of mineral-rich, parasite-free soils. This calls into question how much sodium our ancestors could have safely ingested from this source.
Claim: The author mentions, without citing any references, that “Our ancestors also likely had salt licks and drank rainwater, providing clear evidence that previous estimates of sodium intake during our evolution are most likely drastic underestimations.”
Fact check: According to the WHO, rainwater is “very low in dissolved minerals”. Rainwater samples across multiple countries contained anywhere between 7 and 503 µeq/L of sodium according to this study, which translates to roughly 0.16 to 11.57mg/L of sodium. Even drinking 3L/day of rainwater at the saltiest concentration found would yield only 34.7mg of sodium per day. In other words, not a heck of a lot.
I did not research salt licks in detail, but this British Columbia wildlife guide states that “Mineral licks are relatively uncommon across the landscape.” Africa, where our ancient ancestors lived for millions of years, has been described by researchers as a “salt-poor” continent. While it’s certainly possible that some early humans had access to salt licks, it would seem to be the exception rather than the rule.
Claim: A low-salt diet reduces sex drive and fertility, increases erectile dysfunction, sleep problems, etc.
Fact check: These claims were based on this 2008 article, written by two consultants to the Comité des Salines de France, the French salt trade association. I ran out of time digging through all of the various studies they referenced, though a few seemed to support some of the author’s assertions. However, the cited “Effect of Antihypertensives on Sexual Function and Quality of Life: The TAIM Study” concluded that, when comparing low-sodium to normal-sodium diets, “Responses to the sexual satisfaction subscale, which asks participants how satisfied they have been in the last 6 months with the quality of their sex life, the frequency of sex, the strength of their sex drive, and their ability to be aroused . . . were not differentially affected by assignment to any of the drug and diet combinations for men or women.” In other words, there was no difference between the low-sodium and normal-sodium diets on the quantity or quality of sex.
Claim: “The low-salt-eating Yanomamo Indians average only one live birth every four to six years, despite being sexually active and not using contraception.”—the implication being that a low-salt diet reduces fertility.
Fact check: This claim was backed by a reference to the paper “Effect of Antihypertensives on Sexual Function and Quality of Life: The TAIM Study”, but I could not find any reference to the Yanomamo aboriginals in it. In contrast, Napoleon A Chagnon, an anthropologist who actually lived among the Yanomamo, noted in his book Noble Savages that out of all 171 Yanomamo females of reproductive age (i.e. aged 11-44) that he surveyed at the time, 13 were pregnant and 92 were lactating. In other words, 61.5% of females of reproductive age were either pregnant or had recently given birth. I will leave it to the reader to decide whether the low-salt Yanomamo appear to have fertility problems.
Claim: “Monkeys that groom one another don’t do so to eat fleas, as is commonly presumed—they do it to eat each other’s salty skin secretions.”
Fact check: This 2017 paper “The Number of Louse Eggs on Wild Japanese Macaques (Macaca fuscata) Varies with Age, but Not with Sex or Season” reviews the evidence and states that “Primates also remove harmful ectoparasites, such as ticks and lice, as well as louse eggs, during grooming, e.g., Japanese macaques (Macaca fuscata: Tanaka and Takefushi 1993), chimpanzees (Pan troglodytes: Zamma 2002b), and baboons (Papio cynocephalus: Akinyi et al. 2013).” On the other hand, a former director of the Zoological Gardens of Rome stated that their monkeys rarely got fleas and that they hunted for salt crystals instead. Thus, grooming may have served both functions. In fact, many other functions to grooming can be found with little effort.
Fact check: Earlier societies did not even understand that the heart pumped blood until William Harvey challenged conventional notions in the 1600s. Furthermore, according to the researchers at Encyclopedia Britannica, heart disease “did not become apparent until the 17th century, when examination of the body after death became acceptable.” Based on these, it would be odd to expect reports of heart disease prior to this time.
It was also only in 1912 that American cardiologist James B. Herrick found that the narrowing of coronary arteries could cause angina, a syndrome which had puzzled scientists for centuries. Thus, angina was not interpreted as a clear symptom of heart disease until the 20th century. All in all, it seems unwise to expect accurate, reliable data on heart disease prior to the 20th century.
I also find it interesting that, in contrast to the author’s earlier argument that all humans naturally seek a narrow range of sodium (3,000-4,000mg/day), we are now presented with a large theoretical drop in sodium consumption over a period of centuries. Why? Well, in order to vindicate salt as a risk factor for heart disease, it seems.
Interestingly, in 2015, researchers were able to examine 16th– or early 17th-century hearts preserved in the basement of a French convent, and found that the majority did in fact show significant signs of heart disease such as arterial plaque. “They were really pathological,” according to Fatima-Zohra Mokrane, a radiologist at the University Hospital of Toulouse. Although this is a small study, it certainly casts doubt on the claim that there was little or no heart disease in that era.
Claim: “The Rice Diet was found to dangerously deplete salt in the body, drastically lowering plasma chloride from 97 mEq/L to 91.7 mEq/L. (Bear in mind that chloride levels lower than 100 mEq/L are independently associated with higher mortality.)”
Fact check: These plasma chloride figures do match what Kempner wrote on p.552 of his 1948 report. Various sources list a normal chloride plasma range as either 96-106 mEq/L or 98-106 mEq/L. Either way, the chloride levels did in fact drop below the normal ranges on the very-low-sodium rice diet (about 150mg sodium/day), which would be concerning. It’s unclear if these values would have rebounded after a period of adjustment to the diet or would have remained at such a low level. It’s also unclear how much these low levels were due to heart disease (since they were already low before going on the rice diet), and to what degree these lowered levels would affect health outcomes. I could not find any good information on the impact of low-sodium diets on serum chloride levels, other than infants solely fed chloride-depleted formula or disabled adults being tube-fed low-chloride liquid formulations. The bottom line, however, is that even though the rice diet caused a drop in serum chloride, it still resulted in markedly increased survival rates when compared to normal (sodium chloride-rich) diets.
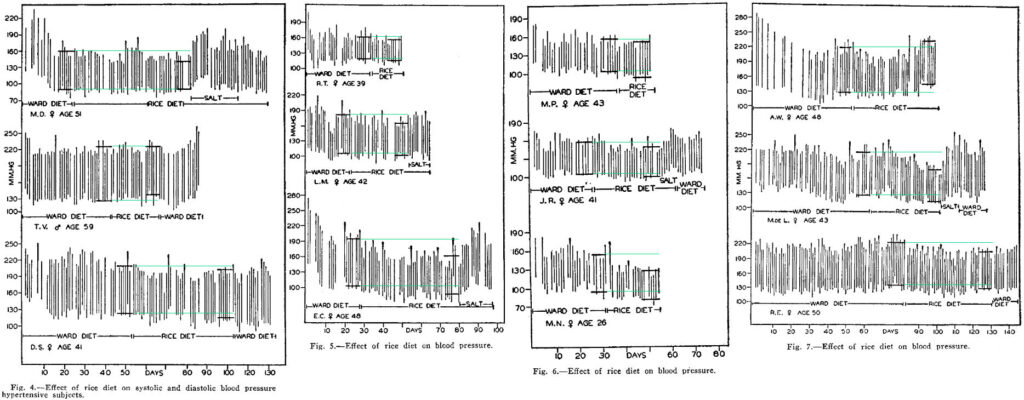
Claim: “In one study of patients with essential hypertension who tried a version of the Rice Diet, 83 percent were found to have no reduction in blood pressure.” And most patients appeared to have reduced kidney function based on various markers.
Fact check: The authors of that 1950 study had a very strict interpretation of “reduction in blood pressure.” They only considered the rice diet a successful treatment if both the SBP and DBP fell all the way down to normal ranges, dismissing all of the lesser reductions in blood pressure experienced by 10 of the 12 patients on the rice diet. See for yourself Figures 4 to 7 below, which show the blood pressure before (on the ward diet) and after (one the rice diet) of the 12 patients—I projected the “before rice diet” readings as green bars to make them easier to compare to the “after rice diet” readings. That said, various biomarkers of kidney function appeared to worsen, perhaps owing to the fact that the rice diet is not just low in sodium but is also very nutritionally unbalanced.
f
Claim: “Only one out of four people is able to comply with rigid salt restriction, making it a rather futile public health policy.”
Fact check: While it’s true that many people struggle to lower their salt intake, the main reason is that the food supply is saturated with salt. Out of convenience, habit, or “addiction”, many of us eat a significant amount of prepackaged or processed foods and these typically contain high amounts of sodium (or added sweeteners, to be fair). For people dependent on such foods because they can’t cook or choose not to, the only effective sodium-reduction strategy isn’t to tell people to eat less salt, but rather to reduce the amount of salt added to processed foods.
Claim: A 1982 sodium-reduction randomized controlled trial led by British cardiovascular researcher Graham MacGregor showed, as DiNicolantonio describes, “mixed results.”
Fact check: Nineteen patients were counseled on how to reduce salt in their diet. Of these, fifteen experienced a reduction in blood pressure, two stayed roughly the same, and a further two (who had the lowest blood pressure to begin with) experienced somewhat of an increase. On the whole, the group experienced a 6.1% drop in mean blood pressure, which the authors note “is in the same range as that produced by a diuretic alone or a beta-blocker alone.” Is it accurate to portray these as “mixed results”? Or is it deceitful? 🤔
Claim: A low-salt diet increases triglycerides, cholesterol (specifically LDL), which are linked to heart disease. “Even the famous DASH-Sodium trial—the foundation of the most well-known low-salt diet—found that salt restriction increased triglycerides, LDL, and the total-cholesterol-to-high-density-lipoprotein ratio (TC:HDL).”
Fact check: The authors of the cited analysis of the DASH-Sodium trial actually concluded that “Overall, the DASH–Sodium trial showed no significant effects of sodium intake on serum cholesterol, LDL cholesterol, HDL cholesterol or triglycerides over a 77 mmol/d range of urinary sodium reflecting achieved intakes of approximately 65, 107, and 142 mmol/L, whether with the control diet or the DASH diet.”
Furthermore, the 2019 US Committee to Review the Dietary Reference Intakes for Sodium and Potassium examined several systematic reviews of sodium’s effects on blood lipids. They noted that, since it can take four weeks for blood pressure effects to stabilize when reducing sodium intake, a similar stabilization period is likely required for blood lipids. “Analyses with the criteria of at least 4 weeks (Aburto et al., 2013; Graudal et al., 2011; He et al., 2013) did not find a significant effect of sodium reduction on total cholesterol, whereas analyses that included studies of shorter duration found a significant mean difference (Graudal et al., 2011, 2017).” Of note, DiNicolantonio chose to only reference the Graudal meta-analysis (that included studies of shorter duration), and ignored the others.
Claim: Salt reduction may cause a potentially dangerous increase in heart rate. The author references a single study by Overlack et al, and asks us: “what has a bigger impact on your health: a one-point reduction in blood pressure or a four-beat-per-minute increase in heart rate?”
Fact check: It turns out that many studies have measured heart rate following sodium reduction. The largest meta-analysis of these that I could find was by Graudal et al (2016), which compiled 72 studies and found a mean increased heart rate of 1.65bpm. However, as we have seen repeatedly, the human body can take several weeks to adapt to a change in salt intake, and this meta-analysis includes many studies less than two weeks in duration, which might skew the results. So, I pooled the studies based on the duration thresholds below and recalculated the mean bpm difference (weighted by sample size). Based on these calculations, we can see that the mean heart rate change tends to decrease as the study duration increases:
All studies: 1.67 bpm HR increase
Only studies ≥ 14 days: 1.08 bpm HR increase
Only studies ≥ 28 days: 0.87 bpm HR increase
Only studies ≥ 40 days: 0.40 bpm HR increase
Only studies ≥ 90 days (i.e. the longest study): 2.00 bpm HR decrease
Claim: The 1991 systematic review by Law et al projected an abnormally large drop in blood pressure of 10/5 mmHg for normotensives and 14/7 mmHg for hypertensives when cutting sodium intake by 2,300 mg per day.
Fact check: What the authors of this systematic review actually wrote was that, in people over 50, a drop of 2,300mg/day would “lower systolic blood pressure by an average of 10mmHg and by 14mmHg in those with high blood pressure. For diastolic blood pressure the reduction would be about half these values.” In other words, the 10/5 mmHg estimate appears to apply only to those aged 50 and up, and to both normotensives and hypertensives combined. It appears that DiNicolantonio misinterpreted the 10/5 figure as applying to all ages and to only normotensives. Misinterpreted in this way, this figure is indeed much larger than what other studies have found for normotensives.
Claim: “Many low-salt advocates argued that salt-restriction trials hadn’t been performed long enough to show a benefit, yet a systematic review of eight randomized controlled trials looking at salt restriction of greater than six months found similarly small reductions in systolic blood pressure (–2.9 mmHg in people with hypertension and –1.3 mmHg in people with normal blood pressure).”
Fact check: That 1998 meta-analysis by Shah Ebrahim and George Davey Smith did result in the above drops in blood pressure. However, the sodium-reduction effects on hypertensives were heavily dampened by the largest included study, TAIM—the only study to find an overall inverse correlation between sodium intake and blood pressure. And the reason TAIM found an inverse correlation was because the control group (the “change nothing” group!) had a highly unusual average drop of -9.6 mmHg SBP despite making no changes whatsoever to their diet and being given only placebo pills. The authors explained that this anomaly may have been partly due to 20% of the patients in the control group having their antihypertensive medication dosage increased during the trial as part of their outside-of-study medical care. The other factor that contributed to this unusual inverse relationship was that many in the low-sodium group failed to significantly reduce their sodium intake, as per their urinary sodium measurements. When the authors looked only at participants who successfully reduced their sodium intake below 1,610mg/day, they found a -23.7/13.9 mmHG drop in blood pressure—a slightly larger drop in DBP than achieved by either of the two medications tested in this trial.
Claim: The 1988 Intersalt study was erroneously used to conclude that salt increases blood pressure. “Only five populations of the fifty-two studied consumed less than 2,400 milligrams daily, and four of them were primitive societies. The fifth population that consumed under 2,400 milligrams of sodium actually had a higher systolic blood pressure compared to several populations with a higher salt intake. In fact, one population consumed more than twice the amount of salt but had a lower systolic blood pressure. And when the four primitive societies were excluded from the other fifty-two populations, the data shifted—suddenly there was a clear downward slope for blood pressure as salt intake increased. That’s right: as salt intake increased, blood pressure actually declined.”
Fact check: Experts know that salt is not the only factor that affects blood pressure, which is why some countries have a higher sodium intake but lower blood pressure (or vice versa). What DiNicolantonio is in effect saying is, “If I selectively exclude data points, I can make the conclusion change in my favour.” The truth is that this can be done with almost any study, but it wouldn’t be very good science. As Intersalt illustrated, very few populations consume low-sodium diets, and deliberately excluding them would give much more weight to all other confounding factors known to affect blood pressure. When the Intersalt researchers included all populations and factored out the known confounding factors (age, sex, alcohol use, BMI), they ended up with an upward slope (i.e. positive correlation) between sodium intake and increased blood pressure (see Figure 4b). Granted, it was not a dramatic upward slope, but it was upwards nonetheless.
Claim: DiNicolantonio criticizes the blood pressure-cardiovascular disease hypothesis, saying, “as we all know, correlation does not equal causation—just because one thing (salt) may sometimes lead to another thing (higher blood pressure), which happens to correlate with another thing (cardiovascular events), that does not necessarily prove that the first thing caused the third thing.”
Fact check: He seems to have no problems with correlations when he states that low-salt regimes cause changes to surrogate markers that he thinks we should worry about: “Appel continued to ignore the harmful effects caused by sodium restriction on numerous other measures of health (called surrogate markers) such as increases in renin, aldosterone, triglycerides, cholesterol, LDL, [etc]”, describing several of these as “factors with much more thoroughly and rigorously documented links to heart disease.” (I have fact-checked these surrogate markers elsewhere.)
Claim: “The sugar industry had other strategies to keep the public naïve to the harms of sugar. In the Supplemental Views to the 1977 Dietary Goals, the sugar industry stated, ‘It should be noted that sucrose (sugar)…does not displace other foods, but rather promotes their consumption. Though often referred to as empty calories, it is really Pure Calories with No Fat and No Cholesterol; . . .’ That’s one Jedi-level mind trick right there.”
Fact check: DiNicolantonio uses the same trick when he says “using salt allows us to consume more vegetables (i.e., potassium), which leads to an overall improvement in our health and blood pressure.” This is a logical fallacy, since salt makes it easier to eat everything—including a large variety of highly processed, nutrient-depleted foods. Salt on its own does not make people choose to eat more vegetables instead of processed foods.
Claim: “Since household refrigeration began in the United States (1911), salt intake has been on the decline. And this would have occurred right around the time a “toxic dose” of sugar was now being consumed in the United States.”
Fact check: According to the USDA “Nutrient Content of the U.S. Food Supply, 1909-2004: A Summary Report”, sodium per capita per day in the food supply has steadily climbed from 920mg in 1909-1919 to 1270mg in the 1960s, then stayed more or less stable (see Table 3). This contradicts the author’s claim that US salt consumption is on the decline ever since the introduction of the refrigerator, which would have helped to vindicate salt as a risk factor for cardiovascular disease.
Claim: “Despite his potential bias and conflict of interest as part of a group [WASH] whose sole focus is to reduce sodium intake around the globe, [Lawrence] Appel was also appointed as a member of the 2005 and 2010 Dietary Guidelines Advisory Committee.”
Fact check: WASH is a registered charity consisting of unpaid volunteers, including hundreds of cardiovascular experts like Lawrence Appel. Their primary goal is to improve population health, and members join because they already believe that high salt diets cause harm. In contrast, the author has no qualms referencing Michael Alderman and John D. Swales without disclaiming that both have ties to the salt industry—whose primary goal is to make money.
Claim: Several countries (South Korea, France, Japan, and others) consume a relatively high amount of sodium yet have low rates of death due to coronary heart disease.
Fact check: There are many factors that impact a country’s mortality rate due to coronary heart disease. First, there are the factors that increase the chances of getting coronary heart disease, which (other than sodium) includes alcohol, smoking, and being sedentary or overweight. Second, there are the factors that reduce your chances of dying from coronary heart disease once you have it, such as access to inexpensive, high-quality medical care. The three countries singled out above, for instance, have excellent healthcare systems which are largely subsidized by government. Cherry-picking individual countries that fit a given hypothesis while ignoring the many confounding factors shows a lack of scientific acumen.
Claim: “[South] Koreans [who eat a lot of salt] manage to somehow have one of the world’s lowest rates of hypertension, coronary heart disease, and death due to cardiovascular disease. This is known as the ‘Korean Paradox’”.
Fact check: From this 2019 study analyzing the 2007-2017 Korea National Health and Nutrition Examination Survey (KNHANES), 51.5% of South Korean adults have either prehypertension or hypertension, including those being treated (see Table 1, % Study population). If over half of the adult population suffers from some form of hypertension, does it make sense to call this a “low” rate of hypertension?
Claim: “In contrast, Latvia, with a salt intake about half that of Japan (7 grams versus 13 grams) has a death rate more than ten times Japan’s.”
Fact check: According to the 2008 WHO report Latvia—Health system review, “Despite rapid economic growth, poverty in Latvia is extensive . . . In general the lifestyle of the Latvian population is unhealthy, due to high levels of alcohol consumption, smoking, unhealthy diets, insufficient physical activity, and obesity. Mortality from diseases of the circulatory system is very high, causing more than half of all deaths.” Latvia also has a poorly-ranked health care system. Singling out salt intake while ignoring the many other risk factors impacting mortality—including poverty, smoking prevalence, alcohol use, inactivity, obesity, and lack of healthcare—makes for a zippy one-liner but isn’t very good science.
Claim: “Here’s the truth: normal blood pressure is less than 120/80 mmHg. But reducing your salt intake to around 2,300 milligrams per day (1 teaspoon of salt) may only lower your blood pressure by a meager 0.8/0.2 mmHg.[16] So, after enduring staggeringly bland and often debilitating salt restriction, your blood pressure may now hover around 119/80 mmHg—a mere blip, not a significant difference. […] even in those with hypertension (blood pressure of 140/90 mmHg or higher), reducing salt intake may only lead to a reduction in blood pressure of just 3.6/1.6 mmHg.”
Fact check: Here’s the truth: the cited 1999 meta-analysis of 114 studies does not mention a drop of 3.6/1.6 or 0.8/0.2. To be fair DiNicolantonio isn’t that far off the mark: the analysis states that hypertensives experienced a mean drop of 3.9/1.9 mmHg, and normotensives dropped by 1.2/0.26 mmHg. More importantly, the author seems to ignore the fact that even a 1 mmHG drop in systolic blood pressure translates to thousands fewer heart attacks, strokes, and other adverse cardiovascular events each year across large populations.
The author also ignores that higher salt consumption is associated to increased blood pressure with age. In other words, present-day normotensives may get away with eating a high amount of salt for a few years (blood-pressure wise), but they’re much more likely to eventually become hypertensives.
Finally, the suggestion that low-salt diets are bland may be true for those used to high-sodium diets, but overlooks the fact that taste buds can adapt to a lower sodium intake. I switched to a low-salt diet back in 2010 and, after a few weeks, all the formerly “bland-tasting” foods started tasting “normal” again.
Claim: “Another consequence of the low-salt diet is that your arteries can become more constricted (an increase in what’s called “total peripheral resistance”), due to the depletion of blood volume. To fight against this increased resistance in the smaller arteries, the heart needs to pump harder, and the pressure of the blood coming out of the heart would need to be even higher. Total peripheral resistance places additional stress on the heart and arteries, leaving you more vulnerable to chronically elevated blood pressure. In other words, low-salt diets may actually cause the very disease they are supposedly being used to prevent and treat, hypertension.”
Fact check: The reference used to back this up was a single four-day study done in 1980. As we’ve seen, short-term salt reductions often produce temporary effects that dissipate over time. Other researchers say that salt can instead increase total peripheral resistance. Furthermore, total peripheral resistance is only one of the determinants of blood pressure, and careful long-term studies show that reduced sodium diets reduce overall blood pressure (as noted elsewhere in this article).
Claim: “When the intake of sodium is severely restricted, blood volume can go down by 10 to 15 percent. This change indicates the body is under stress of dehydration.”
Fact check: I cannot find any reliable source of information indicating that a lower blood volume due to a low-salt diet is a sign of dehydration or is in any other way problematic. The reference he cites actually suggests that a lower blood volume appears to be the norm for modern-day low-salt primitive societies, and that those on a higher-salt diet may actually have an abnormally high blood volume.
Further, the Mayo Clinic states that dehydration is primarily caused by losing more fluid than you take in—not by low sodium intake—and that preventing dehydration involves drinking more fluids—not consuming more salt.
Claim: “Another [rat study] found that eating more salt improved the blood-pressure-lowering effects of metformin.”
Fact check: That study found that if you fed them rat chow containing 8.0% salt (which is about 27x saltier than regular rat chow containing 0.3% salt), and gave them 100mg/kg metformin (which is roughly 3x the maximum dose that you would give to a human, by body weight), then the blood pressure lowering effects of metformin were indeed amplified. Of course, this kind of Extreme Rodent Makeover bears little practical application to human clinical practice. Note that prior to being given metformin, the high-salt diet induced an 8 mmHG increase in blood pressure, and when the rats were given a slightly-less-excessive amount of metformin (50mg/kg), it simply brought their blood pressure back down to pre-high-salt-diet levels.
Claim: “Even weight loss itself had been found to produce large reductions in blood pressure—even when sodium intake was not reduced. […] drop the pounds, and the blood pressure would follow without having to drastically cut salt intake.”
Fact check: Most experts agree that being overweight or obese is one of the risk factors leading to high blood pressure. But that doesn’t mean that sodium isn’t also a risk factor—both are important.
Claim: Various lines of evidence show that potassium has a beneficial effect on lowering blood pressure. Author then concludes that, “rather than look for ways to cut salt, we could seek out ways to eat more potassium-rich plant-based foods, such as leafy greens, squash, mushrooms, and avocados.”
Fact check: Several meta-analyses have found that potassium does lower blood pressure in hypertensives. But again, this doesn’t mean salt isn’t also a risk factor.
Claim: The 2013 report by the Institute of Medicine (IOM)—now called the National Academy of Medicine (NAM)—found that “there was no benefit for restricting sodium intake below 2,300 milligrams per day. In fact, it found that there may be adverse health outcomes. Nevertheless, inexplicably, the original 2004/2005 IOM upper limit on sodium of 2,300 milligrams per day was allowed to stand and ‘remains the basis for federal salt policy today.’”
Fact check: The IOM committee that wrote this report chose (or were instructed to) (A) ignore the abundant evidence linking sodium to intermediate markers (i.e. blood pressure), which in turn were linked to cardiovascular disease, and (B) ignore all evidence of sodium intakes below 1,500mg/day. Could these unusual constraints have something to do with the fact that at least four of the members of that committee had known ties to the salt industry (Michael Alderman, David McCarron, Suzanne Oparil, and Judith Stern), which the author fails to mention? 🤔 Hmmm…
Based on the evidence reviewed within those limited parameters, the IOM committee did not conclude that there was “no benefit for restricting sodium intake below 2,300 milligrams per day” as the author stated, but rather that “evidence from studies on direct health outcomes is inconsistent and insufficient to conclude that lowering sodium intakes below 2,300 mg per day either increases or decreases risk of CVD [cardiovascular disease] outcomes (including stroke and CVD mortality) or all-cause mortality in the general U.S. population.
The potential adverse outcomes of going below 2,300 mg/day were primarily based on a set of studies on patients with heart failure carried out by a single research group (Paterna, Parrinello, Licata). This group was later found to have “fudged” some of their numbers, leading to these two Expressions of Concern and a retraction of a meta-analysis based on them—whose lead author was—drum roll please—DiNicolantonio. DiNicolantonio does not mention that these studies nor his meta-analysis were retracted or flagged as suspicious, choosing instead to continue referencing them e.g. in this editorial
The more recent 2020 PROHIBIT randomized controlled trial placed 21 heart failure patients on either a 3000mg or 1500mg sodium diet for 12 weeks. All meals were provided, and though there was a significant amount of noncompliance to the meals, sodium excretion dropped significantly in the 1500mg group and less so in the 3000mg group. No adverse effects were found. On the other hand, “Quality of life improved in the 1500-mg arm at 12 weeks but did not change in the 3000-mg arm.”
Other potential concerns that the IOM committee raised for sodium intakes under 2,300mg/day included:
⨳ A concern for diabetics was based on a single study which found that (A) feeding genetically modified atherosclerosis-prone mice 10x their usual salt intake would inhibited the RAAS and therefore inhibited plaque formation, and (B) the FinnDiane observational study, which found a J-shaped relationship between sodium intake and all-cause mortality, but suffered from several potential biases including reverse causation (see Thomas et al, 2011 entry in Table 3).
⨳ A concern for those with chronic kidney disease, which was based on two studies, the aforementioned FinnDiane study (which again found a J-shaped association) and a randomized-controlled trial, which in contrast found a linear positive association between sodium intake and adverse renal and cardiovascular events.
⨳ A concern for those who have preexisting cardiovascular disease, based on three studies, two of which found that a high salt diet led to worse outcomes than low salt, and a third study that reanalyzed two RCTs that relied on spot urine and the notorious Kawasaki formula (in other words, not using gold standard 24hr urine collections) and that was criticized for its likelihood reverse causality due to the low-sodium group being sicker and more highly-medicated than the other groups. In defense of this criticism, the study authors replied saying that their results were consistent with other studies, pointing to one of the “fudged” studies by Paterna et al discussed earlier (!).
Claim: Several large-scale studies have found that lower sodium intakes (less than a threshold varying between 2,400 and 3,000mg /day) were associated with a higher degree of mortality. Therefore, an intake of between 3 and 6 grams per day is likely the optimal range for most of us.
Fact check: All of the cited studies received a significant amount of criticism for various methodological flaws. The 2011 study by Stolarz-Skrzypek et al was roundly criticized (for example, see here and here), not to mention that it was co-authored by Jan A. Staessen, who is affiliated with industry trade group The Salt Institute. The 2014 study by O’Donnell et al similarly received significant criticism. And the 2014 study by Graudal et al was also criticized.
Claim: “A low-salt diet may cause you to absorb twice as much fat for every gram you consume.”
Fact check: In healthy individuals with intact bowels, virtually all fats are absorbed before reaching the large intestine—with some exceptions, such as nuts that haven’t been thoroughly chewed. The supporting reference is to a mouse study showing that the more salt the mice ate, the less fat they absorbed—up to half as much. In humans, those who don’t absorb fat properly have medical conditions such as Crohn’s or cystic fibrosis. Since full fat absorption is a feature of a normal, healthy bowel, it make more sense to describe this study’s finding as “a high salt diet impairs normal fat absorption in mice, leading to oily mouse stools and possibly anal mouse leakage.” (Remember the fat substitute Olestra? Shudder.)
Claim: “If you slash your salt intake dramatically, you also could develop an iodine deficiency, since table salt is our best source of iodine.”
Fact check: This is very misleading. First of all, the only reason table salt contains iodine is because the governments of some countries have mandated that it be added to it in order to reduce thyroid disease. Second, the vast majority of the salt that the average person in an industrialized nation consumes is not iodized table salt but rather salt added by manufacturers to foods—and almost none of it is iodized. For most of us, cutting out salt means cutting back on processed/prepared foods and switching to reduced-sodium or unprocessed foods, which will not affect our iodine intake.
Furthermore, the best natural sources of iodine are fish, seafood, and seaweed. Dairy products often contain iodine, though the amount varies based on the amounts added to cattle feed or used to sterilize teats or milking equipment. Rather than getting your iodine from table salt, you’d probably be better off eating foods that naturally contain it. If that isn’t possible, then from a multivitamin.
To be fair, the author changes his mind towards the end of the book, recommending that we “first try to obtain iodine from your diet. . . . [You] should probably not solely rely on iodine-containing salt to obtain your daily iodine intake.”
Claim: “Low-salt diets have also been found to increase liver fatty acid synthesis, which can contribute to nonalcoholic fatty liver disease (NAFLD), commonly known as “fatty liver,” as well as organ fat storage, compared to a normal salt intake”.
Fact check: Sounds authoritative, but this is based on a single rat study. It’s well-known that animal studies are often poor predictors of human outcomes. Scientists need to replicate these results in human studies, multiple times, in peer-reviewed journals, by independent research teams before they can responsibly make authoritative claims like these.
Claim: “[If] someone exercises for an hour, they may lose around 2 grams of sodium, so their intake would need to be higher in order to replace what was lost.” (No references are cited)
Fact check: Based on thousands of sweat tests done by Precision Hydration, “some athletes lose as little as 200mg of sodium per liter of sweat, while around 20% of athletes lose more than 1,500mg/L”. Those on a low-salt diet eventually excreted as little as 75mg sodium per litre of sweat, based on experiments done in hot environments with and without physical exercise, which increased significantly after going back on a high-salt diet. This experiment also showed that working unacclimatized in searing 50C heat caused at most 1.5kg (1.5L) of sweat produced per hour. By combining the previous numbers and using the worst possible conditions, an unacclimatized individual exercising for an hour in extreme heat and sweating at the maximum rate may lose as little as 112.5mg sodium per hour and a minority may lose in excess of 2250mg. So while it is true that a minority of us in these extreme conditions may lose around 2g of sodium per hour, for the vast majority of us who are exercising in moderate temperatures, excreted sweat and sodium will likely be much lower. As confirmed by the World Health Organization, “Even in hot, humid climates, there are only minimal loses [of sodium] through faeces and sweat. Acclimation to heat occurs rapidly; thus, within a few days of exposure to hot and humid conditions, individuals lose only small amounts of sodium through sweat. Under conditions of extreme heat and intense physical activity that result in high sweat production, sodium losses in sweat are increased and appreciable; nonetheless, most individuals can replace the necessary sodium through food consumption, without dietary alterations, supplements or specially formulated products.”
Claim: “It’s not too much salt that creates “salt addiction.” It’s salt restriction, which increases our risk of salt depletion, that can [. . .] cause the brain to get a greater reward or “high” from salt. These modifications resemble the changes that occur in people who have become addicted to drugs of abuse, and this sensitization can be hijacked by other substances of abuse. Sounds amazing, doesn’t it? [. . .] But the evidence in the literature strongly supports this notion. [. . .] by making the brain’s addictive pathways more sensitive, salt restriction likely also makes people more susceptible to dangerous addictive drugs and food addiction.”
Fact check: “Sounds amazing”? Or “sounds ridiculous”? He overlooks that his own reference speculates that “Salted Food may be an addictive substance that stimulates opiate and dopamine receptors in the brain’s reward and pleasure center”. Even if low-salt diets augment the reward value of amphetamine or cocaine, what the author fails to realize is that it likely augments the reward value of everything in life, not just drugs of abuse. I have personally experienced this when I cut most salt out of my diet: all other foods began tasting better (i.e. their “reward value” increased). Crucially, I did not suddenly turn into a drug addict—I merely started enjoying everything more.
Claim: “Studies have noted that a low salt intake in pregnant mothers may cause offspring to eat and crave more salt throughout childhood and adulthood.”
Fact check: Wait a sec, I thought the author said we all had a reliable “salt thermostat”? This claim is based on a review of rat studies, and its author noted that a high-salt diet also led to offspring consuming more salt. Another review of rat studies found that “attempts in rats to relate early sodium intake to long-term salt preference have yielded inconsistent results” and that the same was true for studies of infant and childhood exposure on later salt preference. However, they did find that vomiting in pregnancy or in childhood increased the child’s salt preference several years later. So there are indeed some early-life factors that appear to alter an individual’s salt preference years later.
Claim: “A 2011 study from the University of Haifa in Israel suggests that a high salt intake may help buffer the effects of stress, serving as an adaptive coping mechanism for dealing with psychological and emotional adversity.”
Fact check: This was based on a rat study funded by the Salt Institute, a major trade association for the salt industry. Draw your own conclusions.
Claim: “Similarly, researchers at the University of Iowa found that when rats are deficient in sodium chloride (table salt), they shy away from normally enjoyable activities, suggesting that salt has a positive effect on mood.”
Fact check: Another day, another rat study. The authors of this one also noted that our “physiological and behavioral means for maintaining body sodium and fluid homeostasis evolved in hot climates where sources of dietary sodium were scarce. For many reasons, contemporary diets are high in salt and daily sodium intakes are excessive [and] can have pathological consequences.” DiNicolantonio seems to have glossed over these points.
Claim: “Low-salt diets can cause tremendous sacrifice and general misery for those who attempt to follow them. Pines and colleagues have even suggested that low-salt diets may induce serious anxiety, hypochondriasis, and invalidism. In other words, people feel anxious and ill on low-salt diets.”
Fact check: Though I am only a case study of n=1, I feel better on a low-salt diet than when I used to be on a higher-salt diet. Furthermore, Pines et al seemed to be speculating when they wrote in this 1949 paper that “The required environmental and psychological adjustments [to a low-salt diet] may induce serious anxiety, hypochondriasis and invalidism”, since they did not back up these statements with any references nor does the rest of the paper mention any of these points. Referencing one sentence of idle speculation from over 70 years ago? Not terribly scientific.
Claim: “Once upon a time, our taste for sweet foods was functional because it ensured that our ancestors would consume enough calories and nutrients from naturally sweet foods like berries and other fruits. But in our modern food supply, the natural sugar from whole foods has been extracted and stripped of its inherent fiber, water, and phytonutrients until all that’s left is a refined white crystal or chemically produced syrup. Unfortunately, this sweetening does not generally result in an increased consumption of fruits or sweeter vegetables—but rather an increased consumption of refined sugars.”
Fact check: Hmmm… 🤔 What if we rewrote the above paragraph this way (see if you can spot the differences): “Once upon a time, our taste for salt was functional because it ensured that our ancestors would consume enough sodium from natural sources like unseasoned whole meat, fish, and vegetables. But in our modern food supply, the natural salt from the ocean has been extracted until all that’s left is a refined white crystal. Unfortunately, this salting does not generally result in an increased consumption of fruits or vegetables—but rather an increased consumption of processed foods.”
Claim: Processed foods containing large amounts of refined sugar “stimulate the brain’s reward centers, causing them to light up on PET scans like pinball machines, just as addictive drugs like heroin, opium, and morphine do.”
Fact check: Processed foods containing large amounts of salt also stimulate the brain’s reward centers—think cheese, potato chips, pizza, hamburgers, deli meats, and French fries. If you remove all of the salt, how good will these taste? You can test this yourself if you can locate unsalted chips, unsalted cheese, unsalted popcorn, or make your own fries without any salt (nor other salty seasonings, of course). Then compare the salted and unsalted versions side by side to see which one “lights up your brain’s reward centers.”
Claim: Sugar gives a larger reward than addictive drugs (see table Shared Features between Addictive Drugs and Sugar).
Fact check: Have we jumped the shark yet? Have you ever seen a homeless sugar addict strung out on a downtown sidewalk? Me neither. I am not in any way saying that added sugars are healthy, but let’s be realistic. The authors of his cited study do conclude that sugar binging leads to many neurochemical and behavioral changes similar to drugs of abuse, but “[the] effects we observe are smaller in magnitude than those produced by drug of abuse such as cocaine or morphine”.
Claim: Hypothyroidism can lead to hyponatremia, so we may need to consume more salt. (No reference is provided.)
Fact check: This 2015 paper reviewed the evidence: “In conclusion, in more recent years, the paradigm that routine cases of hypothyroidism cause hyponatremia has been challenged. Outside of severe cases of hypothyroidism, particularly those referred to as myxedema coma, hyponatremia of clinical relevance appears dubious. […] routine hypothyroidism as an etiology of hyponatremia is unlikely”.
Claim: A variety of people in inpatient and outpatient settings have varying rates of hyponatremia (unusually low blood sodium levels). The elderly are more impacted: “Hyponatremia is also found in 18 percent of nursing home patients […] One has to wonder if the low-salt meals that many nursing home patients are served as a matter of course are contributing to this pattern.”
Fact check: The author is painting the picture that we should all eat more salt in order to prevent hyponatremia. According to ye olde Mayo Clinic, the root causes of hyponatremia include various diseases (like those of the heart, liver, or kidney), various medications (such as diuretics), severe vomiting and diarrhea, hormonal imbalances, and simply drinking too much water. Having a low-salt diet is simply not one of the root causes. Yes, consuming salt (or receiving an IV saline solution in a hospital) can certainly help to correct a sodium imbalance after the fact. However, treatment for hyponatremia generally involves targeting the above root causes rather than simply eating more salt. To borrow the phrasing of the author, one has to wonder to what degree the high-salt meals that many sick patients have eaten for their entire lives has contributed to these various diseases.
Claim: Sweating during exercise can cause dehydration, tremors, muscular weakness, and even cardiac arrhythmias, cramps, fatigue, and hyponatremia.
Fact check: Regarding symptomatic hyponatremia, his own reference (Tim Noakes) reviewed the literature and concluded that “There is no evidence that, in the absence of fluid overload, the usual sodium deficits generated during exercise can cause this condition.” Hoffman et al compared the sodium intake of 20 ultramarathon finishers with the various symptoms they experienced during the race and concluded that “Exercise-associated muscle cramping, dehydration, hyponatremia, and nausea or vomiting during exercise up to 30 h in hot environments are unrelated to total sodium intake, despite a common belief among ultramarathon runners that sodium is important for the prevention of these problems.” However, Sawka et al found that in ultra-endurance events lasting over four hours, sodium losses through sweat could potentially cause symptomatic hyponatremia regardless of over- or under-drinking, and that in these specific cases replacing the sodium losses was warranted.
Claim: “For example, in animals, low salt intake during pregnancy and/or lactation leads to increased fat mass, insulin resistance, and raised levels of “bad” cholesterol and triglycerides in the offspring, which may carry over into adulthood. More worrisome is that a low-salt diet in pregnancy has also been found to cause hypertension and kidney disease in adult offspring. All of this suggests that low salt intake during pregnancy may program our children to develop abnormal lipids, diabetes, obesity, hypertension, and chronic kidney disease—the very diseases we believe a low-salt diet will prevent!”
Fact check: These claims are based on four rat studies. Why look at rat studies when we can look at human studies? This 1995 Dutch study of low-salt diets effects on 41 pregnant women (with matched controls) concluded: “No significant effects of a low sodium diet on infant birth weight, placental weight or other pregnancy outcome variables (length and head circumference of the infant, Apgar scores and arterial pH of the cord blood) were found. In the present study, the prescription of a low sodium diet in pregnancy resulted in a reduced intake of energy and several nutrients. Nevertheless, the pregnant women appeared to be able to adapt quite well to this reduced intake, since calcium, zinc and magnesium homeostasis was maintained. Also, no effect on infant birth weight, considered to be the best measure of the quality of pregnancy, was found. Therefore, the results of the present study give no reason to advise against sodium restriction in healthy well-nourished Dutch pregnant women.” Add to that this study on 476 infants that showed that lower sodium intake in infancy lead to a mean 3.6/2.2 mmHg lower blood pressure 15 years later (in the 167 children they could track down).
Claim: “As we age, our levels of renin and aldosterone are reduced, and with them, our kidneys’ ability to retain salt, increasing our risk of salt deficit.”
Fact check: While it’s true that the elderly generally have lower levels of renin and aldosterone, their overall kidney function is slower at both re-absorbing and excreting sodium. Given a sodium load, it takes longer for elderly individuals to get rid of the excess sodium. And when switching to from a higher-salt to a lower-salt diet, it takes their kidneys longer to adapt and start reabsorbing the sodium they would normally excrete. This means that greater care must be given to the elderly when either increasing their sodium load or decreasing it, and when starting—or altering the dose of—medications that may affect their sodium balance.
Claim: “If you have salt-wasting kidney disease, you may require more than 6 to 7 grams of sodium per day to maintain stable kidney function. If you cut your sodium to 1,610 to 2,300 milligrams of sodium per day, you could promptly become severely ill because of low blood volume and compromised kidney function.”
Fact check: The author is basing the prescribed sodium amounts on a case study of a single patient back in 1965. If you are diagnosed with a specific disease that causes a sodium imbalance, then you should follow your doctor’s prescribed advice. This may include starting new medications, altering existing medications, making changes to your diet, and yes, consuming more or less salt. However, this does not mean we should all start consuming more salt “just in case.”
Claim: Because the intestines can selectively reduce sodium absorption, and the kidneys can selectively reabsorb less sodium, and excess sodium can be stored in our skin and other areas for later use, “the human body is well adapted to handle salt overload—but not salt deficit.” On the other hand, a low-salt diet causes our body to be in a “state of emergency” and “panic” and increase our levels of renin, angiotensin, and aldosterone hormones.
Fact check: The human body also has mechanisms to handle sodium deficit, which are essentially the opposite of those for high sodium. This includes our kidney’s ability to reabsorb over 99% of the sodium passing through it, which is moderated by the renin-angiotensin-aldosterone system (RAAS) of hormones. To paint the high-salt adaptation mechanisms as “well adapted” but the low-salt adaptation mechanisms as a panicky “state of emergency” are entirely subjective characterizations designed to fit the book’s narrative. It is much more accurate to say that both sets of mechanisms are essential to maintaining the narrow, optimal range of sodium in our blood. Look to the other evidence to decide if low-salt versus high-salt is the healthiest choice instead of relying on biased characterizations.
Claim: “Sodium restriction is particularly harmful in chronic kidney disease because hyponatremia is extremely common (13.5 percent).”
Fact check: As mentioned earlier, the root causes of hyponatremia include various medications and diseases, as well as severe vomiting and diarrhea, hormonal imbalances, and drinking too much water—not low-salt diets. This 2018 meta-analysis of eleven randomized controlled trials found that “moderate salt restriction significantly reduces BP [blood pressure] and proteinuria/albuminuria in patients with CKD [chronic kidney disease].” And since elevated blood pressure and proteinuria are both risk factors for kidney disease, this means that moderate sodium restriction actually improves CKD outcomes.
Claim: “Caffeinated beverages, acting like natural diuretics, can increase water and salt loss from our kidneys.”
Fact check: A number of studies do show that sodium excretion increases by about 50% after consuming 400mg caffeine (the equivalent of roughly 4 cups of coffee). It isn’t clear to what degree this impacts those on a low-sodium versus a higher-sodium diet. In the absence of further evidence, if you drink many caffeinated beverages each day and are already on a very low salt diet, you may want to consider consuming a little more sodium—or a little less caffeine.
Conclusion
DiNicolantonio wraps up The Salt Fix by asking us to challenge all those who rely on conventional low-salt wisdom to back up their assumptions with evidence such as high-quality studies. The author has indeed drawn from a large number of studies to convince us that the higher-salt diets consumed by most countries is not only harmless, but beneficial. However, many of them are of low quality: rat studies, case studies, observational studies with known confounders or poor methodology, short studies that did not give the body time to adapt to a big drop in sodium, idle speculation from decades ago, and even studies that he clearly knows have fudged their numbers (those of the Paterna group). But two wrongs don’t make a right. Likewise, a large number of poor-quality studies do not add up to good quality evidence.
If a non-PhD-wielding layperson like myself can arguably dismantle (or at least cast serious doubt on) the bulk of the author’s arguments with about three weeks of concentrated effort, what does this say about the quality of the research behind this book? We should ask ourselves: is it possible that the author has accidentally overlooked all of the scientific evidence countering his claims, which I did not have too much trouble locating? Or is it more likely that the evidence was selectively chosen and selectively interpreted in order to fit a pre-determined narrative? 🤔
Furthermore, what does it say about the various doctors that have given glowing back-of-book reviews, including neurologist David Perlmutter, chiropractor Josh Axe, physician Michael R. Eades, and cardiologist Aseem Malhotra? Have they critically examined the book’s contents? Have they even read the book? 🤔
An interesting pattern emerged as I dug through the various lines of evidence. There appeared to be a cluster of anti-low-salt researchers centered on the Albert Einstein College of Medicine in New York—a cluster including Michael H. Alderman, Sylvia Wassertheil-Smoller, Albert Oberman, Hillel W. Cohen, Susan M. Hailpern, and Sean Lucan. It is known that some of these researchers have taken money from the (now defunct) Salt Institute trade association. And we can link DiNicolantonio to this cluster as he has worked extensively with Sean Lucan. Statistically speaking, what are the odds that so many independent-thinking scientists in one college all have exactly the same unorthodox, pro-salt opinion? The last time I saw a cluster like this was in a group of pro-saturated-fat doctors working out of Duke University. I later discovered that Duke’s nutrition programs had received several multi-million dollar grants from Atkins Nutritionals, the maker of popular high-fat, low-carb bars and other snacks. Coincidence? 🤔
James DiNicolantonio is certainly right about one thing: do not accept everything you are told as a fact—including both the claims in his book and the counter-evidence I have put forward. Check the evidence and decide for yourself.
Bda, bda, bda, that’s all folks! Thank you for reading—I hope you enjoyed it (and maybe learned a few things along the way). Have any suggestions or criticisms? I look forward to hearing from you below. To your health!
50 replies on “Fact-checking The Salt Fix”
Great work on fact checking “The Salt Fix”. Three weeks of solid work, you have my thanks.
Thanks Colin! I invested my time in this “high salt versus low salt” fact-checking article to (hopefully) save other people from going through all that the trouble themselves. Take care.
Pierre
Much obliged to you for this work! I must admit to owning the book & it persuading me to increase my salt consumption (& have indeed benefited from doing so) but I was not very convinced by the author’s many claims. You’ve just shown me I was correct to be sceptical. That said, I’m not about to radically reduce my salt intake from what it is now (5-10g of table salt a day) because I’ve yet to be convinced that this level of consumption is detrimental to me. But I’m quite content with scientific uncertainty & less content with false certainty gained by cherry-picking data to suit, as you have shown, was clearly done by the author. (I’d given up following him on Twitter a while ago because of this tendency.)
Glad to have helped! The best thing any of us can do is try to look at *both* sides of a debate and then make up our own minds. After all I’ve read, I’m still convinced that for most people, 1,500mg sodium (or 3.7g) sodium or less is the ideal range, but I have to admit that some people may need more depending on genetics, health status, lifestyle, etc. Curious to know in which ways a higher-salt intake helped you! Cheers…
Not table salt most studies are from intake of table salt which is refined poisonous trash . Redmonds real Celtic any that come from nature . I like Redmonds because it contains (natural) forms of iodine . This forum is trash to begin with . IMO
Sodium chloride is sodium chloride. Legitimate studies that resulted in negative salt cardio results were not based on salt with additives or anti-caking agents. Any scientist would laugh at such a blunder. With that said, there are plenty of pure salt products on the market, of which Redmond’s contains among the highest in lead according to testing results such as mamavation. Redmonds is also involved in some kind of legal action regarding false claims.
Celtic (which is just an expensive form of French gray salt) also contains higher than normal levels of heavy metals, possibly due to the man-made clay beds it is harvested from.
You’re an example of ppl who believe everything the industries throw at you (and the people supported by them, like DiNicolantonio).
This was phenomenal. Came across his Instagram recently and was very surprised at the huge popularity he had gained. He posts what seems to be (at best) commonsense or (at worst) deeply misleading commentary on nutrition and health.
Your rebuttals to his book confirm what I had strongly suspected, and saved me from doing the work myself!
Thanks Marian! Glad to have saved you some trouble. I tried to stay open to changing my mind when examining The Salt Fix, but it became quite clear to me that the evidence had been selectively chosen (or selectively interpreted) to support his hypothesis that we should all eat a higher-salt diet. And at the same time, much of the (rather easily found) high quality evidence supporting lower-salt diets had been deliberately omitted. And that is not real, honest science. Cheers!
A deep thank you for this research! You have saved me from having to read the Salt Fix book itself. I am already rather skeptic several pages into the book, but do not have the time to check its claims myself. Luckily I don’t have to because lo and behold, an Amazon review refers to this page. Keep up the good work.
I’m glad you found this fact-check useful! Sharing my findings so that others did not have to replicate this effort was one of my goals. Cheers!
Fantastic, Pierre. Thank you. I’ve had a deconstruction of this book on my to-do list for some time, but haven’t gotten to it. Funnily enough, despite your thoroughness, I still have additional criticisms!
Thanks Amber! If you have more critiques/criticisms of the book that you think I should integrate into this review, feel free to pass them along. If I add them in I will credit you for them, of course. I didn’t spend too much time on the “sugar” side of the book, but I’m not sure if that was your area of interest. Cheers!
Hi!
Do you have a link to the research article on those renaissance mummy hearts? The CNN article isn’t helpful to find the primary source. Only thing I’ve found looking into the mentioned authors is a CT scan of a mummy that was found to have no vascular lesions in what remained of its arteries.
https://link.springer.com/article/10.1007%2Fs00414-018-1830-8
Hi Harmless Frog! I tracked down the study, which is entitled “Old hearts for modern investigations: CT and MR for archaeological human hearts remains
“. The abstract can be found at https://www.sciencedirect.com/science/article/abs/pii/S0379073816304029?via%3Dihub . Also, here’s an excerpt from the full paper:
“Various investigative techniques permitted normal and pathological findings. Except for heart n°2 (too damaged) and n°3 (subnormal), all other specimens appeared to suffer from heart disease. Heart n°1 was hypertrophic and all ventricle walls were thickened. Histology showed cardiomyocyte hypertrophy associated with an expansion of the collagen network. These findings confirmed the pathologic character of this heart, consistent with diffuse hypertrophic cardiomyopathy. Heart n°4 showed several signs of dilated cardiomyopathy: dilated ventricles, decreased wall thickness, and an increased collagen network. The radiological exploration of heart n°5 was impossible, because of intentional post mortem opening and extensive lead infiltration. However, it showed severe histological abnormalities with an extensive expansion of the collagen network. These findings may be consistent with secondary dilated cardiomyopathy accompanied by severe fibrosis, without providing evidence of its origin.”
And this excerpt:
“Atherosclerosis is commonly considered to be a disease of modern man and related to modern lifestyles. However, evidence of atherosclerosis was found in different mummies, like Egyptian, ancient Peruvian, North American but also in Tyrolean iceman[44–46]. Most of these lesions were diagnosed using CT, by evidence of calcified plaques[47]. In our cases, atherosclerosis was diagnosed using its consequences: a later narrowing of the vessel’s calibre. This was possible using coronary opacification, and confirmed by histology.”
I’ve not read the above review yet, but I have an experience to share.
I ate a very low amount of sodium for years and years. I am aware of salt in canned food, etc. I am taking all of that into account.
My sodium intake was perhaps around 200 mg per day.
I read The Salt Fix and thought maybe this was a key part of healthy eating that I was missing. The book also made me wonder why I was not sick or dead, having eaten so little salt for so long.
I upped my intake of Himalaya salt to 1/4 teaspoon, with dinner.
I could feel the new higher amount of pressure inside my body. I figured it was fine. Keep in mind, all I added was about 550 mg. of sodium, taking me up to maybe 800 mg per day max.
I finally decided to take a break from the extra pressure (blood pressure) and skipped the added salt last night.
I may just be more sensitive to salt than most, but I wonder if that is just my body no matter what, or if it is because I went so long with so little sodium that my body became amazingly efficient at using what it got. (If indeed I am more sensitive to salt than most.)
I am not saying I do not need more sodium. I am saying my blood pressure, according to my experience and feeling of it inside of my body, went up.
I cannot even imagine how I’d feel eating 2,000 mg of sodium per day.
Is it possible I can be healthy with 200 mg per day?
Hi Barry! Thanks for sharing. Yes, it is possible to be healthy by eating only 200mg sodium per day. The INTERSALT study found that the Yanomamo aboriginals of Brazil consumed on average around 23mg (!) of sodium per day and were in generally good health (Source: https://www.nature.com/articles/srep11123) Keep in mind though that, living in primitive conditions, they did not generally have access to medical care and so were more vulnerable to infections, etc, and it is these kinds of things that tend to shorten their lifespan. That said, some people may have specific medical conditions or genetic traits that require them to eat more sodium. But the average healthy person can easily live with less then 500 mg/sodium per day, and likely a lot less than that. The human body adapts to lower sodium diet by holding on to more sodium in the kidneys and sweat glands. If you have done well so far on a 200 mg sodium per day diet, I would not worry about eating too little sodium unless your doctor advises you to eat more for specific reasons. Cheers!
From the abstract: Contrary to this hypothesis, C57BL/6J mice fed a 45% high fat diet exhibited weight gain that was inhibited by increased dietary sodium content.
This study you sourced is about mice.
Yes, the study I referenced in my above comment is about mice. But in the “Discussion” section of that mouse study, the authors talk about the Yanomamo aboriginals of Brazil consuming around 23mg sodium/day.
You are right though that I probably should have referenced a more direct source such as https://iris.who.int/bitstream/handle/10665/43738/9789241595935_eng.pdf . Cheers…
Yes, the study I referenced in my above comment is about mice. But in the “Discussion” section of that mouse study, the authors talk about the Yanomamo aboriginals of Brazil consuming around 23mg sodium/day.
You are right though that I probably should have referenced a more direct source such as https://iris.who.int/bitstream/handle/10665/43738/9789241595935_eng.pdf . Cheers…
I read the article in full.
Thank you for putting in the time to do that.
Hello, I have skimmed through your site and do agree that not all research is good. I do think that doctors give bad advice because they are indoctrinated not to offend they coorporations that fund their organizations, so I think there is a lot of research out there that is suspicious.
With all the crap that we use to preserve our food I think salt is one of the healthier options and I think the western world would be healthier going back to it.
Thanks for the work.
Thanks Pierre. A lot of work, and much appreciated. I remember reading “Salt, Diet and Health” by MacGregor and Wardener years ago, which included a comment about a UK prime minister (John Major) getting advice from health advisors that reducing salt in the food chain would significantly reduce premature deaths in the general population, but that he was talked out of implementing legislation towards that end by salt industry lobbying, so when I saw the publicity about “The Salt Fix” I was sceptical. But didn’t have the time (or skills) to do the fact checking. Again, thanks, and best wishes from Scotland.
Thanks David! My goal in publishing this article was indeed to save other people the time and trouble of fact-checking the dozens of claims made in The Salt Fix, or at least give them a good starting point to do their own fact-checking. Cheers from Canada. 🙂
Thanks Pierre!
A great work! When I saw the title of “Salt fix” I was excited. I have been eating massive amounts of salt (don’t even ask) for years and thought it would give me some justification at last. Well, I see it won’t. And thanks to you I will be more careful with letting loose my addiction.
Thanks for the feedback Marek! I used to eat a lot of salty foods too, even salty drinks (which many people found gross). Cutting back was hard, but the amazing thing is that taste buds do eventually adapt so that you don’t miss it anymore. Take care from Canada. 😊
I showed my Salt Fix-believing brother this page, and it immediately made him see the truth.
Just kidding. He called this debunking “BS”, without reading it. His existing Salt Fix-belief was reaffirmed.
As for me… I won’t be wasting my precious time on this book, myself!
Well, at least you tried showing this to your brother. 🙂 I find it interesting when people shoot down evidence without even looking at it… I’ve seen the same happen with anti-vaxxers, like Del Bigtree calling several studies (which contradicted his beliefs) “bad science” immediately after first hearing about them, without even ever having looked at the abstracts, let alone the details. Take care…
This is all good and well. But let me say. I had a slight increase in my flat intake. My BP systolic went up up up. Dr said ok we need to put you on BP tablets that made my diastolic pressure increase. He say ok take twice the dose. Hmmm it was already making me feel really sick. So based on what I was taught too much sodium cause high Bp and hardening of arteries I though ok. So no more salt. I cut salt out of my cooking and diet generally. Result I got sick again. So I had a bit of salt and half an hour later was feeling so much better. We have to get the balance right.
I have a new Dr who said if especially on Keto diet must have some salt. So now I am having small amounts of salt and feeling so much better!!
Thanks for sharing your experience, Lyn. When you say you got sick again after lowering your salt intake, what were your symptoms and how long did you try the lower-sodium diet? When I cut way back on my salt and sugar (I dropped both at the same time), I had flu-like symptoms for a week, then fatigue on and off for another 10 weeks, but I really hated the idea of going back to my old diet so I just kept going. After the 10 week mark, I finally felt back to normal. So, for me at least, it took a while to feel okay again. That said, I’m not doing keto and I’ve heard that people on keto may need more sodium, at least for the first few weeks of the diet. Cheers…
as a general practitioner and sport medicine physician I can say following the salt fix philosophy of increasing the salt intake of the athletes i’m taking care of led to better performances, they all report feeling better, better stamina, less injuries and contractures etc…
i’ve also seen improvement on digestion for people with low stomach acid. the effects on low cortisol and thyroid hormones i can also confirm. it literally cures POTS almost every time.
in my experience it only messes up with people who are metabolically compromised, yes if you increase sodium intake on an insuline resistant patient his blood pressure is going to rise. on the other hand, when patients are willing to decrease their sugar consumption increasing salt intake helps them fighting cravings and eating less.
try fasting with or without drinking a salty drink also, you’ll feel much better with the salty drink. (more energy, less headaches)
your debunking was interesting to read but anyone can try lowering the sugar and increasing salt and witness the effects on himself very quickly. (chose a good quality salt of course)
if salt restriction for high blood pressure worked it would allow to get the patients off their medication, i’ve never witnessed that. it’s the other way around, they need more meds… that’s not “the science”, that’s just what I see. maybe you should let your wife try it, it made sense to her, maybe she’ll feel better with less carbs and more salt. I do. most “the salt fix” readers do. why not try like a week or two?
Merci d’avoir partagé tes pensées, Dr. Buono! Of course, if a particular individual feels better (or performs better) in the short term on a higher salt diet, I cannot refute it. And there are certainly some specific conditions that warrant a higher sodium diet (I had not read about this for POTS, thanks for sharing). However, I would also be concerned about the long-term consequences as one’s daily average sodium intake climbs beyond the 2,000mg, 3,000mg, or 4,000mg levels–sodium intake levels that are nearly impossible to achieve on a natural diet of plain, unprocessed whole foods (with the exception of shellfish-heavy diets). Some of the studies I’ve cited show that high-sodium diets are associated with increasing blood pressure with age, which may be due in part to some kind of gradual kidney degeneration caused by the salt. For instance, this 5-year study of roughly 12,000 patients which showed a significant correlation between high salt intake and future kidney degeneration (based on eGFR measures) (source: https://www.karger.com/Article/Fulltext/492406). I agree that lowering sodium is usually not enough to normalize someone who already has developed very high blood pressure, but if it’s enacted early in life, it may prevent someone from developing high blood pressure in the *future* (and thus reduce their risk of heart disease, heart attack, and stroke). Take care. 😊
Thank you so much! People like you make the world a better place.
Thanks Max for your kind words! Hopefully this salt fact-check helps a few people out there…
I was told by this book by a friend whom i was arguing with and telling him that i have genetically high BP and i consume little salt to keep my BP lower even with it being higher then the average person. I read some of this man’s book and saw an interview of him on Youtube. I came across your comment on Amazon under reviews. Many thanks for the research and i will be sure to forward this to my friend and tell him he’s been duped.
I’m glad that you found this salt fact-check useful. I hope that your friend takes a look with an open mind. If either of you find any mistakes or omissions, I will gladly do my best to address them. Cheers…
OMG… My own opinion is that it’s indecent, to say the least, that such types of books not only exist, but receive so many attentions when, as you’ve clearly shown, are full of misleading theories.
Thank you SO much Pierre for the work you’ve done and the time you’ve put into this very high quality fact check!
It would be awesome if you could do the same for many of the other highly biased books out there, in the meantime thank you again, really appreciate your help!
Thanks for the feedback! I wish there were more serious repercussions for scientists who spread misinformation (knowingly or not) that can potentially lead to serious illness and premature death.
Feel free to suggest books that should be fact-checked, though I may or may not have the time. The ideal book would be one that’s fairly high-profile, has the potential to cause serious injury, and hasn’t already been thoroughly fact-checked. Take care. 😎
You did a great job debunking The Salt Fix. The author, in my opinion is a Tucker Carlson of the medical world. He knows better, but outlandish, unsubstantiated claims sell more books.
Let me add another critique to your list. Dr. DiNico asserts with confidence that Nutcracker man also ate a diet largely composed of unnamed species of grasshoppers (p. 24), but he does not tell us what the alleged salt content of the grasshoppers was. Instead he tells us the sodium of content of a different insect, namely, the cricket, but does not identify what species. There must be hundreds if not thousands of cricket species, so we cannot assume they all are equally high in sodium. However, that is not what the author alleges Nutcracker man ate—he ate grasshoppers allegedly, whose sodium content the author does not disclose. But based on that sleight of hand, the author wants the reader to conclude that Nutcracker man consumed a staggering amount of sodium because crickets, which Nutcracker man did not eat, are high in sodium.
Thanks Anna for taking the time to read this fact-check and for pointing out the switcheroo regarding the grasshoppers. Indeed, according to the 2021 paper “Edible Crickets (Orthoptera) Around the World: Distribution, Nutritional Value, and Other Benefits—A Review”, the sodium content of crickets can range from as little as 1mg to as much as 453mg per 100g dry matter, depending on the species. This review also points out that, out of all insects, crickets contain the highest sodium content, which may explain why DiNicolantonio honed in on crickets’ sodium content rather than grasshoppers’. Source: https://www.frontiersin.org/articles/10.3389/fnut.2020.537915/full
Me again. I did not write the last sentence in my above comment, namely: “Your comment is awaiting moderation.”
I do not know how it got there. Disregard it, please.
Hi Pierre,
Just thought I’d throw my two cents in. For the past 2 years I was having quite a few issues with health. Just to put things in context first. I have been active my whole life. Lifting and cardio consistently. I eat a very healthy diet but looking back it was very low in sodium. Something I never even thought about before. Some eggs, fish, fermented foods lots of veg and occasional meat. Olive oil and nuts. I am also someone who sweats a lot. Training and sauna5-6 days a week.
Some years back I started having issues with a higher baseline feeling of anxiety and tolerance to stress which I was normally very resilient against, went way down. Sleep suffered and then about a year ago I started getting frequent PVCS. Needless to say this was not great. I then started to investigate some possibilities. Went to the doctor to get bloodwork done and doctor said everything was fine. all the results were optimal according to him.
I then asked him to send on the results and when I looked at them my salt was one point above what would have been considered low. That got me thinking and searching. I found this: https://hubermanlab.com/using-salt-to-optimize-mental-and-physical-performance/
And then I came across the book you have fact checked. All I can say is its helped me a lot (podcast and some info in book). My PVCS are gone for the most part from hundreds a day to one or two a week. I feel less anxiety and I’m sleeping better which of course compounds the benefits.
I think the key take for me is the benefits are real but it must be done with a healthy natural foods diet. I have read quite a bit of research and for me sugar is hands down the biggest danger to human health not salt. Inflammation is the main driver of disease and when it comes to salt/sugar, sugar hands down is the biggest culprit.
Of course too much of anything is bad but if you look at the salt when considered in the correct way is very important. I highly recommend the podcast by Dr. Huberman – neuroscientist and a great communicator of science. He explains how we have evolved to sense salt and why the brain has dedicated so much effort into keeping this critical mineral in balance.
I wish you a great day.
Thanks for taking the time to write, Michael. Kudos to you for being consistently active (something I need to work on)! Yes, I watched that salt-based episode by Andrew Huberman. Please correct me if I am wrong, but it sounds like you not only increased your sodium intake but have also cut back on added sugars. If so, cutting back on added sugars is one of the best ways to reduce anxiety, and since anxiety is one of the risk factors for PVCs (premature ventricular contractions), this may have been one of the pathways that helped resolve your PVCs. I’m not saying that eating more salt did not help either, mind you. I am entirely open to the idea that some people just need more sodium than others, either due to their current health conditions, their lifestyle (significant sweating, as seems to be your case), their age, or certain genetic predispositions. However, I don’t agree with the core premise of The Salt Fix that *everyone* does best on a ~3,500mg sodium per day diet—the majority of the best evidence I have seen suggests that most people are healthiest on less than 1,000mg sodium per day, and probably need even less than that. Cheers… 🙂
Hei Pierre,
I agree there are a lot of factors to consider. I done a quick check and can say for quite a long time I was averaging 500mg sodium a day. which for me seemed to be way too low. I am at 2500-3000 now. I will also point out my blood pressure is very good and metabolically I’m good. The only sugar I really eat these days( the last 10 years) is dates, dark chocolate and some fruit. I also eat usually in a 6-8 hour window everyday with occasional fast. What I think personally may have tipped the balance(negatively) for me was a change in my life circumstances. There is for sure a relationship between cortisol and sodium and of course the effect stress will have on electrolyte balance. I speculate that I simply hadn’t enough sodium in my diet to keep my electrolytes balanced with all the extra stress.
Of course I cant be 100% sure of anything but that’s where I’ve landed as this moment. It’s worth pointing out that life is like that. We all need to find the right balance for ourselves and remember there is a lot of variation in life. We all have to take responsibility for ourselves and figure out the best we can what works and to do so while being absolutely honest with ourselves. That’s the hard part:) !
Michael
Hey Michael, thanks for sharing! I’m glad you’ve found a diet that works for you. You are right, we each have to tinker with what we eat/drink because our bodies and life circumstances are all different. Cheers… 😎
Thank you for doing all this work!! Now I don’t have to read the book, haha. It’s a real shame that a guy who spreads so much misinformation and so blatantly cherry picks his data has so many people singing his praises. That being said, I am personally in the camp that salt isn’t the bad guy it’s made out to be.
I’d never paid attention to my sodium intake before, but on average it had to be fairly low. I generally follow a whole food diet, put a “normal” amount of salt on my food, and rarely eat processed foods or snacks. I avoid buying chips even though I hear them calling to me when I pass by in the grocery store because I know I struggle to stop eating them. In fact, even though I have avoided processed food and sugar for many years and thoroughly enjoy my healthy, whole food meals, I still find myself craving the unhealthy stuff frequently. I also struggle with chronic fatigue. I am often low energy, low motivation, and even when I’m feeling alright, I tire extremely fast. All I want to do every day after work is go to bed. According to my doctor, everything looks good and I am healthy, but I don’t FEEL healthy.
Fast forward to a few weeks ago, a friend mentioned using electrolyte packets in her water at work because plain water didn’t cut it (she works in a very hot environment) and I immediately had this intuitive thought pop into my head: “You need that.” Very unscientific, but I believe in body wisdom, so I started using more salt and supplementing with electrolyte drinks and within just a couple days I had more energy than I have had in as long as I can remember, and those energy levels have stayed up since. I wake up feeling like a real person, I come home from work and still have energy to do things in the evening, even after really long, exhausting days. And I was very surprised to find that my cravings for salty and sugary junk foods? Gone. The snack aisle holds NO appeal to me.
That’s when I started doing some research and discovered there’s quite a bit of controversy when it comes to salt. I found The Salt Fix and was drawn to it because some of his claims are things I experienced myself, and I read so many people’s accounts of more salt dramatically improving their health, including fatigue like mine. I’m disappointed his research is so biased but I can’t deny the impact increasing salt has had on me.
In my opinion, dietary guidelines should be more broad and nutrition needs need to be assessed more closely on an individual level. Every person is different. I understand the desire to create simple rules that can be recommended to everyone, but that can cause harm to people whose needs fall outside the recommendations (I’ve read many stories of ill folks who were told “limit sodium” by their doctors because that is the convention, but it turned out that increasing sodium is what resolved their symptoms in the end). I think it’s equally harmful to propose everyone limit salt or everyone increase salt.
There is no one size fits all in nutrition and needs can change even on a daily basis. That’s why I am also a huge believer in listening to one’s body. You eat less salt because you feel better that way, I eat more salt because I feel better that way.
Thanks for sharing, Ellen. Yes, certain people may need more salt than others for various physiological reasons, perhaps even a lot more salt. If you feel more energetic by adding electrolytes and salt to your food / drinks, then it would seem to be a strong indicator that your body needs more of these than it was previously getting (though keep in mind that something other than dietary deficiency may be causing this electrolyte imbalance). That said, the research I have seen strongly suggests that *most* people are consuming too much salt and that it is harming their heart / cardiovascular system, their kidneys, as well as increasing the risk of cancers of the digestive tract. Salt also appears to promote overeating and weight gain in most people, which is a risk factor for many other diseases. Ultimately though, you are right that each person is different and that general guidelines don’t always provide the optimal advice for any particular individual. Take care. 🙂
[…] JUNE 2021: Check out Fact-checking The Salt Fix for a deeper dive into the claims made in the […]
DiNocolanto appears to be the love child of Big Salt and Big Food.
Thank you for your honest and thorough fact check. I wonder how many ppl are being injured through DiNocolanto’s financially-driven agenda?
I’m surprised at how many influencers are jumping on his industry-sponsored studies and hailing salt as the answer to circulatory issues as if it’s fact. This is definitely helping weed out the so-called health influencers who lazily parrot others, from those in the same field who do their own due diligence and might question this guy’s study references. It’s certainly helping me clean out my sub list, lol!
As evidenced by the popularity of DiNocolanto’s book, people can easily be manipulated into believing that a food they love, but have (wisely) been told can be harmful to their health in excess, is ACTUALLY a “health food” and can, and should, be used liberally—in daily amounts that are 2-3x the recommended amount. What a joyous relief, right? Next time a concerned wife pulls the salt shaker away from her husband who is already suffering from heart disease he can indignantly cite some of the studies from DiNocolanto’s book and continue to kill himself, unaware the studies were either industry-sponsored, weakly done, or even retracted.
In addition to now being free to liberally over-dose themselves with table salt, folks, once concerned about the high levels of sodium added to processed foods to make them taste good, can now justify enjoying processed foods again ad lib! I’m just waiting for the sugar industry to manipulate the data that donuts are actually a “health food”! 😂
Add to this the popularity that DiNocolanto’s book pushes back against mainstream science. (Which should he noted that, in a rare instance of unbiased studies over 100 years, managed to get it right regarding the over-use of salt.) Science became justifiably distrusted thanks to the likes of Fauci and our own health agencies, so pushback is hailed as a rebellion against the Man. But the public misses the fact that DiNocolanto is leading a rebellion against good science in this instance, while being a mouthpiece for Big Salt and Big Food with whom he has known historical financial ties.
Pretty ingenious how the industries framed this and are driving the success of his book with a big middle finger toward the market of people who normally scrutinize everything they eat. I guess the giant food industries get the last laugh here.
Great job with your fact checking, very much appreciated!
Thanks for your comments, Leslie! Yes, people love hearing good news about their bad habits, unfortunately.
Such a positive and encouraging article. The real-life examples were my favorite part. This is one of the best posts I?e read lately.